My post about trauma-informed care and integrating it into hospital culture posted on KevinMD today! So happy to have the opportunity to raise awareness about best practices in approaching clients coping with crisis and trauma. What was the team approach like at your NICU? Was there anything specifically positive or negative about it? Really enjoying conversations about how we can manifest positive relationships between patients and providers. Have a read here.
Making Memories During Difficult Times: Remembering as a Way of Coping in the NICU
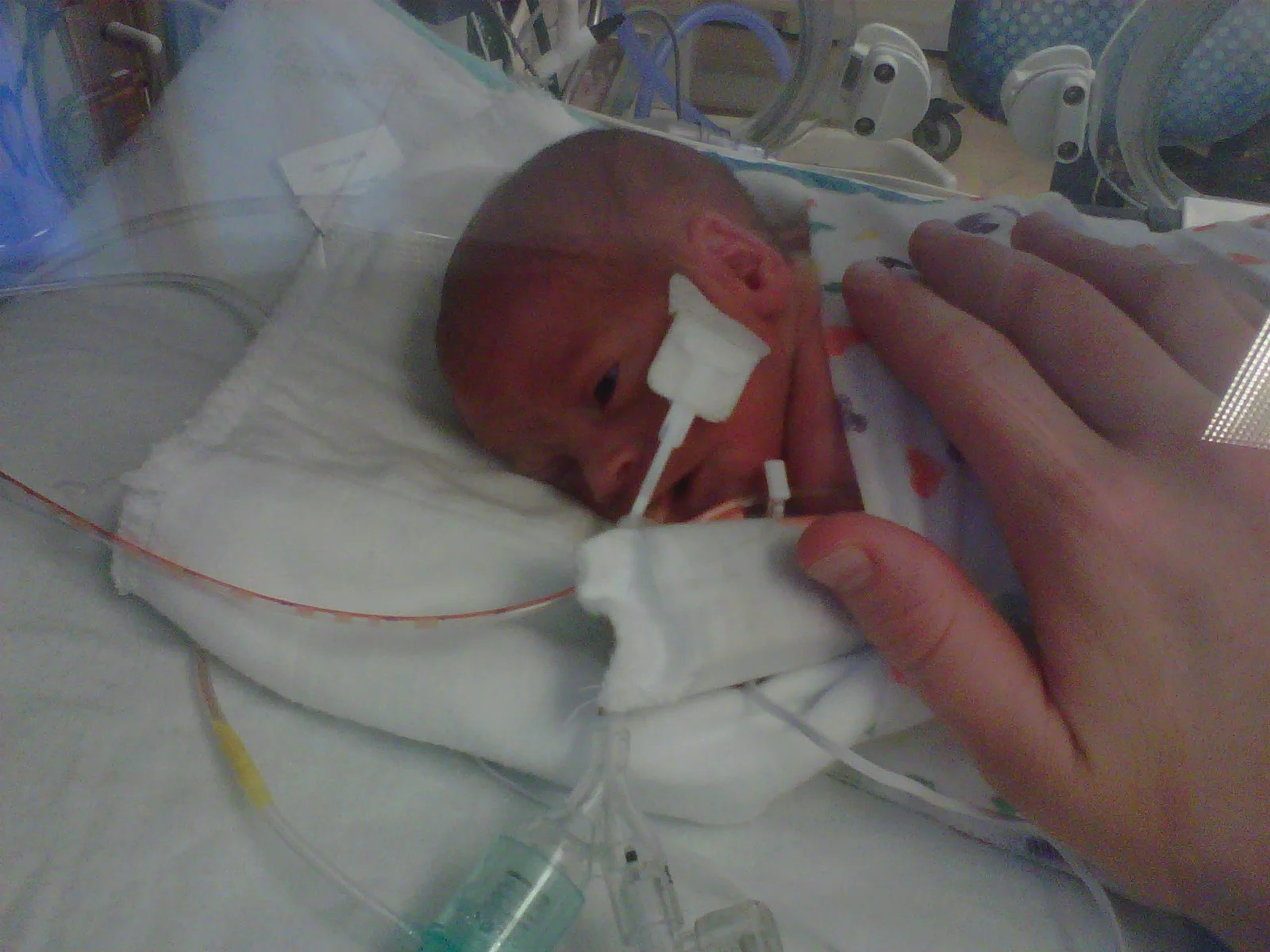
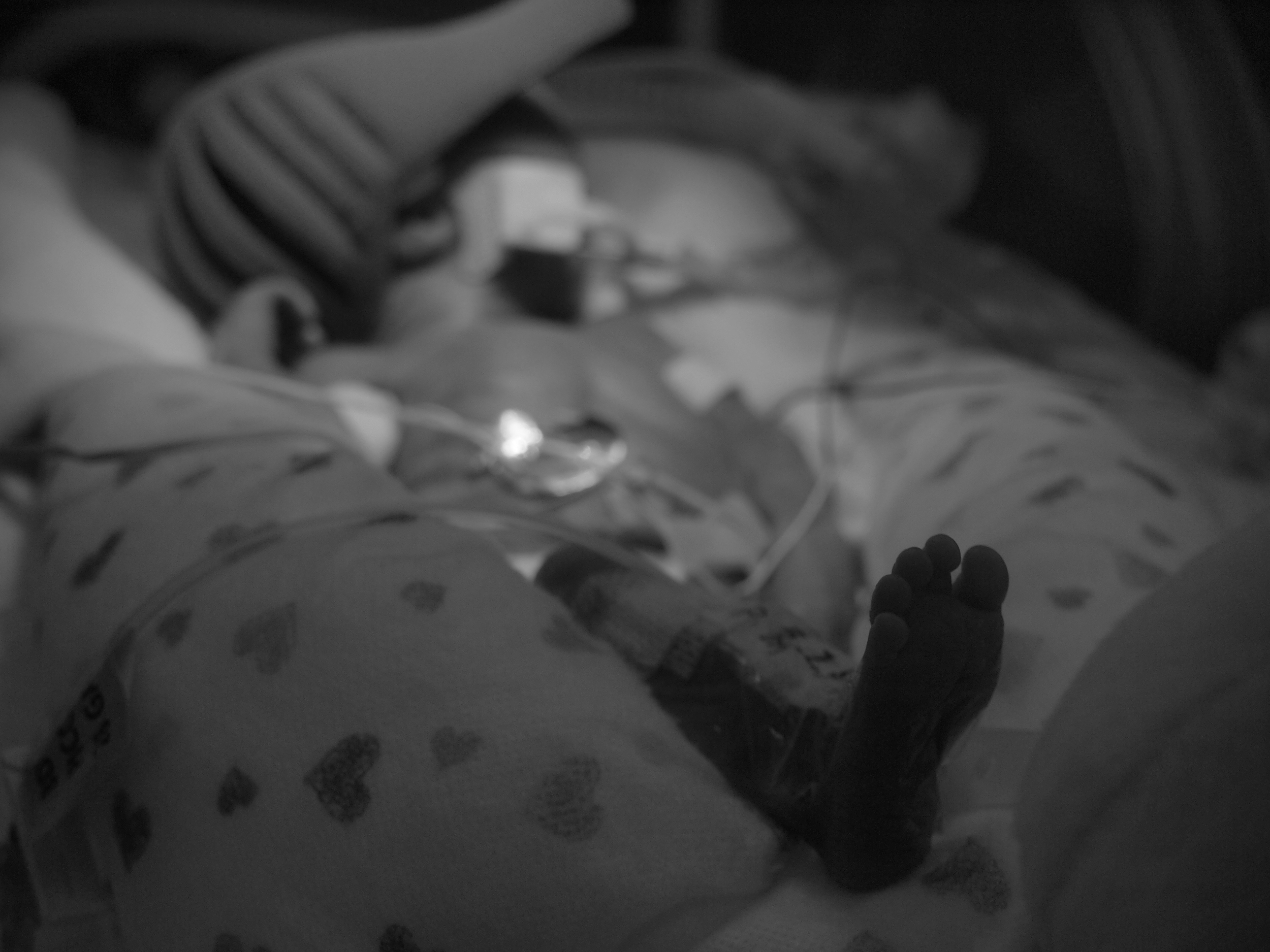
During the first few days of my sons' lives, I was so sad, so overwhelmed, my life so upended and my anxiety level so high, I didn't want to remember it. I remember distinctly thinking, "I don't want to remember any of this at all". At the time my logic was, "why would I want to remember seeing my boys in pain, hooked up to monitors and fighting for their lives? Why would I want to remember what it feels like during what seems to be the worst days of my life?"
Phone photo of Elliott on the ventilator.
It wasn't until after we got home from the NICU and I made connections with other NICU parents that I realized this was a somewhat common experience, however guilty and shameful it made me feel while we were still in the hospital. Even if parents didn't necessarily feel they didn't want to remember the experiences at hand, many are so overwhelmed by the sudden changes in their lives that they don't have the presence of mind to even think of things like taking photos.
What saved me from having a huge gap in my visually-documented memory were a few experienced, emotionally intelligent nurses who made sure that plenty of photos were taken, even when William's health failed, and who further encouraged us throughout Elliott's stay to document all of his little milestones, as painful as they might have been for us. Because of these incredible individuals, our family has pictures of the good and the bad, the horrific and the beautiful, and of each difficult step forward that we took together, and some of the steps backward.
The NICU can be stunning in its complete takeover of what most parents once thought would be a predictable, beautiful experience: the birth of their baby. The first milestones you witness in the NICU are often those that are in their own ways tragic, if only because they are necessary. Getting off of the oscillating vent, being allowed to hold your baby, nippling, being big enough to wear clothing, transitioning from the isolette. These things are very different than what most of us imagined would be the first milestones; things like smiling, reaching for toys, rolling over, milestones that will likely be many months away for a baby who still has weeks before his/her actual due date or who is struggling with medical issues that prevent them from being able to focus on those actions.
Current trauma research shows that in the healing of trauma, it is important for a person to have an integrated, autobiographical understanding of just what happened. In fact, it's common in all kinds of trauma for individuals to have a response similar to what mine was initially: to want to forget, to deliberately disengage from the experiences at hand, to "shut-down" so to speak. However, research is showing that it's just the opposite that will help us to process trauma in a meaningful way. In thinking about this, I realized that creating a coherent, autobiographical understanding of the NICU had another benefit: helping me to someday explain to Elliott what his first few weeks and months were like, the people that loved him, and to show him the images of his beautiful brother.
Here are a few tips for those new to the NICU, who may be struggling with the exhaustion and stress that the experience brings:
1. Take pictures, a lot of them. As hard as it is to see your baby hooked up to wires, bili lights, monitors, and in an isolette, some day, most or all of these things will be a remnant of the past. This post from Hand To Hold is a wonderful tutorial about artful ways to take photos in the NICU, written by a professional photographer and preemie mom. Even in a circumstance where you may be coping with loss (as we did), take as many photos as you can with your baby. As heartrending as it may be in the moment, some day the photos you take will become precious.
2. Get a lovey for your baby to do size comparison pictures each month. Some NICUs provide babies with loveys, or small stuffed animals to comfort them. Taking a picture to document your baby's growth each month will astound you due to what appears to be astronomical growth (and ultimately for micropreemies, really is!). This is an incredible way to watch your baby grow at their own pace, independently of any charts, and to see how far they've come. It's also a great practice to continue after your baby's discharge from the hospital and through the first year.
This small poster from EverytinyThing has space on its balloons for each member of your baby's care team to write their name.
3. Take pictures with your baby's primary nurses, doctors and therapists. Get one of the fantastic products over at EverytinyThing so that your baby's team can write their name on your "My NICU Family" print. The people you see every day at the NICU may seem like they are unforgettable, but years later it can be difficult to remember each of your baby's caregivers and put a name to the individuals that had such a profound daily impact on your family's lives. The isolette decorations that Trish sells can also brighten up your baby's isolette and make the space less daunting.
4. Keep a journal. Journaling not only documents each of the things that happen in your day to day NICU life, but it can also serve the important purpose of making you feel better. Journals can help you express and process your emotional response to different circumstances, if simply by providing a space for you to "get it out". I'd like to emphasize that it's important for dads to write about their experience as well. Again, journals not only serve the purpose of providing a distinct memory of the experience for parents, but can also be something of value in telling the NICU story to your baby when they get older, or in sharing with friends and family about what happened. Personally, in revisiting my journal from my babies' NICU stays, I realize just how strong we actually were, and how easy it is to forget what a struggle it once was.
5. When in doubt, ask your primary nurses for suggestions. Through their experience, nurses have a good sense of the types of things a family can do to generate memories during difficult times. One thing our nurses did for us was take prints of both of our boys' feet and hands (there are some creative ways of doing this that are worth checking out as well!). They also took pictures or wrote notes each time Elliott had a milestone when we weren't there (I still have the note a nurse wrote when he completed his car seat test in the middle of the night!). Additionally, collaborate with your nurses about the things you'd like to have done in a specific way (for example, the first outfit you'd like your baby to wear and letting the nurses know you would like to be there for it).
Many of the practices I took up in the NICU in order to create memories of the circumstance have ended up becoming valuable to me in life after the NICU, particularly journaling. Even though some of these practices may be difficult to fathom in a challenging moment, or may feel unnatural just due to the fact that you've never done them before, have faith that many of them will prove their worth and hold their worth long after your baby's NICU stay is over.
Stay tuned~ a giveaway of EverytinyThing's "My NICU Family" print is coming to NICU Healing's Facebook page soon! Follow our Facebook page to receive updates!
How to Find a Therapist
My guest blog at NICU Central posted today; it's about becoming an informed consumer when seeking out clinical help during or after the NICU. So great to collaborate with such an awesome provider and NICU nurse. Check it out for tips in finding a therapeutic collaborator in making sense of the NICU:
The NICU experience; words to describe it. Terrifying, stressful, saddening, maddening, traumatic, disempowering, fearful, unpredictable, scary, mystifying, changing, bizarre lights, jarring sounds, life and death, tubes, new languages, new people, infection, struggle, adjustment, exhaustion, the unknown, the unexpected, lack of time, too much time, stress, fear, fear, fear. Simply using word association to describe the experience brings back the sensation of being in a new place, not knowing the outcome of any minute, of constantly being reminded that nothing is promised and that there's no way of knowing what tomorrow (or even the next hour) might bring. The words fall short of aptly describing the circumstance, but can give a slight sense of just how destabilizing a traumatic birth experience and the subsequent hospitalization of your baby can feel for a NICU parent. I know because I was one... (Read more at NICU Central)
Mourning a Loss that Doesn't Quite Have a Name: Grief and Loss in the NICU
I just published my first blog for Hand To Hold last week. This is such a fantastic organization with whom to be involved. Looking forward to writing more articles for them about the intense journey and self-discovery of a NICU parent. Check it out here.
Trauma: Why Does There Always Have to be a Reason?
Many parents feel a significant amount of guilt and/or shame after going through a traumatic birth experience and the hospitalization of an infant. One of the most salient conversations I had at the NICU was with one of my sons' neonatologists, who told John and I to be gentle with ourselves. He said we would likely have thoughts, lots of them, desperately examining every detail of the days leading up to our babies' birth, trying to figure out what we did wrong to cause my preterm labor. He was correct. In fact, we had already gotten started researching what it was that made us absolutely responsible for the traumatic birth of the babies. Because how could such a horrific and devastating event happen for no reason? Maybe it was something I ate at dinner, maybe when I moved that piece of furniture a few days ago. Should I have taken a leave of absence at work? Was I too stressed out? Moving. Life events. Did my pets somehow give me an infection? Maybe I wasn't mindful enough. We must have done something wrong.
Traumatic stress, so it seems, often rolls into our lives hand in hand with guilt and shame. Guilt and shame are so common in the experience of traumatic stress that at one point they were considered as potential diagnostic criteria in the classification of post-traumatic stress disorder. Individuals facing other forms of traumatic stress also oftentimes take up the practice of self-blame in the aftermath ("what was I wearing that prompted him to assault me?"). So what gives? Why is it that when an individual goes through a traumatic experience, it's so common to then manifest shame, self-blame and guilt? And what do we do with that? Why is it so hard for us to sit with the notion that sometimes things happen for no known reason?
Psycho-evolutionary theory holds that an individual feels shame and guilt much in the same way an animal might, indicating to the community around them that they have been harmed and need help (Harman & Lee, 2010). So, maybe when we feel responsible for a tragic event, it's our unconscious way of "performing" our trauma for our community, exhibiting our remorse so that we aren't excommunicated. Fair enough, but what if shame and guilt are holding us back from functioning in our day to day lives? What then?
Learn about your circumstance.
Chances are, there was nothing that you could do to prevent your birth experience from going the way it did. Nothing. This is a great article describing some of the most common pregnancy complications, and how despite how much progress has been made in the business of caring for premature or medically complex babies, the medical community still doesn't know exactly what causes these things to happen. Yes, there are risk factors that can lead to complications. However, most of these risk factors are not things that you can avoid. We often hold the assumption that the medical community has expert knowledge of all ailments we might face. Unfortunately, even though so much valuable research and progress has been made in preventing pregnancy complications, many elements are still little understood.
2. Be aware of cultural attitudes that may be causing you harm.
All too often in our society, the unexplainable is not accepted. I was shocked when reading through comments on articles about the World Health Organization's recently released infant mortality and prematurity statistics, to see that many individuals who had never experienced anything remotely like preterm birth had pert answers as to why they felt infant mortality is still an issue in the U.S., offhandedly blaming mothers and families for their own tragic circumstances. Try to shield yourself and your family from these kinds of attitudes, whether in the media or in your own community. When someone asks "What did you do that caused this to happen?", redirect them to the research that shows that you did nothing wrong. If that attitude persists, set a boundary with that individual to protect yourself.
3. Develop a sense of loving-kindness towards yourself.
This is the tough one. How can we move ourselves from a place of guilt and shame to one in which we hold compassion for ourselves and what we are going through? One trick I learned through my own experience was to try and imagine myself from another person's perspective, even my babies' perspective. What might that other person see? Was I doing the best that I could given my current set of circumstances and the knowledge that I had? If I had known some way of preventing this event from happening, would I have done it? By looking in from the outside, sometimes your strengths and values become more apparent. When you start to see and identify your strengths and values, you will also start to develop the ability to grow loving-kindness for yourself. If imagining yourself through the eyes of another person proves to be difficult, start by using affirmations (it's simple to google free affirmations; peruse them and sort out a few that resonate with you). Simply repeat the affirmations either silently or out loud multiple times a day. It may feel alien or strange at first, but sometimes going through the motions of self-reassurance can jump-start the process to reaching the "real" thing.
4. Promote loving-kindness of the self in your partner.
Your partner (or other individual who provides you with significant emotional support) will likely be mired in the same struggle with guilt and shame that you are experiencing, even if his/her struggle looks completely different from yours. When coping with a trauma together, try to be gentle with your partner. Remind them of their strengths or the things that you appreciate about them. Check in with them about how they are coping, even if it seems like you've already addressed all the issues together. In doing these things, you will set a precedent of support in your relationship, and create a space in which you can address the various stresses you're both facing.
Shame and guilt are oftentimes the uninvited guests to an already traumatic event. Allowing these emotions to take over can increase your risk for developing acute or post-traumatic stress disorders (Barr, 2010; Harman & Lee, 2010). If your sense of shame and guilt is so overwhelming that you feel powerless against it, it may be time to seek out counseling.
As our neonatologist continued in the conversation that day, he told us his NICU experience spanned decades. He told us that if the birth were our fault, he would surely tell us. He told us he almost never saw patients that had done something that "caused" their pregnancy complications. He told us that tons of research is being done to prevent this very thing from occurring. That if they could resolve preterm labor and other reproductive complications, that he and his colleagues would be unemployed. "Happily unemployed." His words resonated with me. In fact, for months I would deliberately replay what he said in my mind when I started to develop new theories of why our circumstance was all my fault. To this day, I feel gratitude for what he said.
References
Barr, P. (2010). Acute traumatic stress in neonatal intensive care unit parents: relation to existential emotion-based personality predispositions. Journal of Loss and Trauma, 15: 106-122.
Harman, R. and Lee, D. (2010). The role of shame and self-critical thinking in the development and maintenance of current threat in post-traumatic stress disorder. Clinical Psychology and Psychotherapy, 17. 13-24.
Leskela, J., Dieperink, M. and Thuras, P. (2002). Shame and posttraumatic stress disorder. Journal of Traumatic Stress, 15:3. 223-226.